Diabetes in Children and Young Adults
- The predisposition to diabetes observed in South Asians is apparent even in children and adolescents. Family history is a strong predictor of diabetes in children as is true of adults. 1, 2
- The prevalence of diabetes is 14 times higher in Asian children than white children in the UK where South Asians comprise only 4% of the population, but comprise 24% of the diabetic children and adolescents in the country.3, 4
- In the UK, the increase in childhood obesity and overweight rates are steeper in South Asian children, who were 45% more obese than Caucasian children.5 Furthermore, second and third generation South Asians appear to have many of the same diabetes and CVD risk profiles as their ancestors, and the tendency towards insulin resistance, is already evident in childhood despite a lower BMI.6
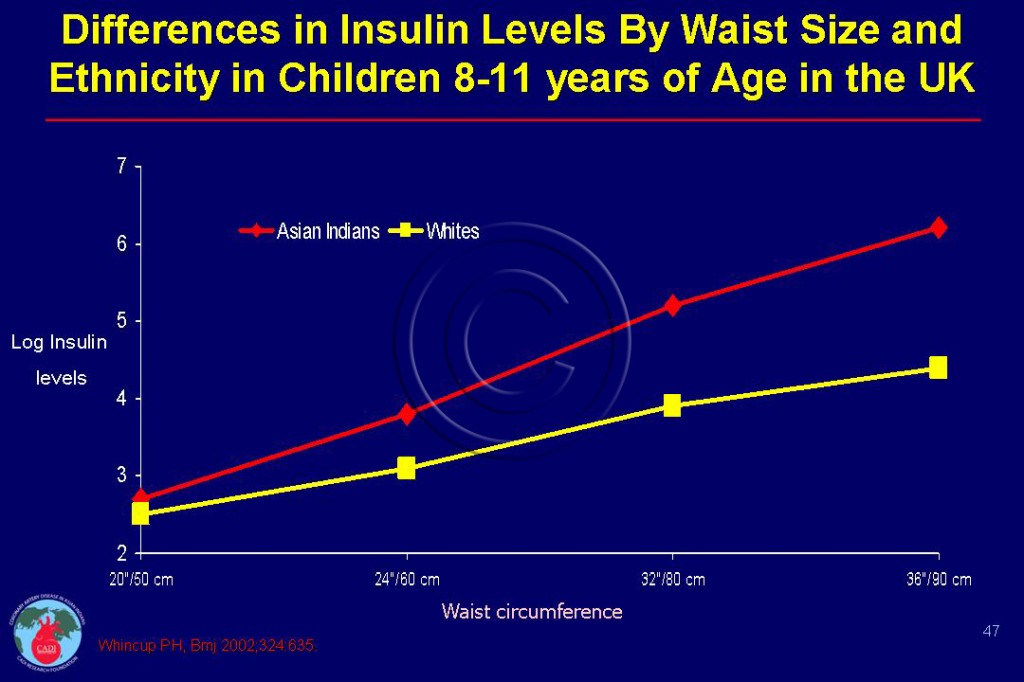
- At a given waist circumference (WC) Indian children 8 to 11 years have double the insulin level than whites─ a tell tale sign of diabetes risk (Figure 047).6 These children also have high triglyceride and fibrinogen levels than white children and indicates a genetic predisposition to diabetes.6
- Insulin resistance is common and appears to be the principle driver of diabetes in children and adolescents.1
- The intrauterine environment experienced by offsprings of diabetic mothers increases diabetes and cardiovascular risks. This effect appears to be greater than genetic factors and the effects strengthen during childhood.7
- Clinical markers of insulin resistance include increased body mass index (BMI), WC, high triglycerides, low HDL-cholesterol, and acanthosis nigricans. The presence of these predictors of cardiovascular risk would translate to cardiovascular disease (CVD) in young adulthood. Hence, diabetes needs to be recognized early in Asian Indian children.1
- Cardiometabolic abnormalities described above are present in young, healthy, Asian-Indian adolescents (n=2,640) and even among those with normal weight. Such abnormalities are found in 65% of normal weight and 85% of overweight children. These findings indicate a large reservoir for diabetes in Indian adolescents.8
- Early identification of diabetes in young Indians is feasible with the simple clinical, anthropometric and biochemical parameters. Predictors of diabetes in children and young adults include family history of diabetes, abdominal obesity, and high triglyceride. The presence of all three risk factors increased the risk of diabetes by 112-fold.9
- South Asian adolescents are more insulin resistant, with more visceral fat than white European adolescents, which may contribute to their increased risk of developing diabetes.10 Levels of physical activity are lower in South Asian children that may further increase the risk.11
- Children in South Asia have a low incidence of insulin dependent diabetes mellitus (IDDM) but migrants to the UK have similar overall rates to that of Europid children (13 per 100,000 for both). However, a more steeply rising incidence is seen in the South Asian population (7% South Asians, and 2% for non-South Asians). This indicates that incidence in South Asian children may eventually outstrip that of the non-south Asians. Genetic factors are unlikely to explain such a rapid change, implying an influence of environmental factors in disease etiology.12
- IDDM is generally believed to be genetic in origin with environment playing minimal or no role; Indian children appear to be an exception to this general rule.
- A study of 614 patients who developed diabetes (< 20 years) from South India found that the age at onset was 11 years in urban patients and 18 years in the rural group. Furthermore those with higher family income (Rs> 2000 /month) showed a sharp peak at 11 years whereas the lower income group showed a peak at 18 years.2
- Although the exact cause for the delayed age at onset of IDDM in the rural or low income group (LIG) is not known, it is likely to be a consequence of the lower socioeconomic and nutritional status as indicated by low body weight.2
Sources
1. Nandkeoliar MK, Dharmalingam M, Marcus SR. Diabetes mellitus in Asian Indian children and adolescents. J Pediatr Endocrinol Metab. Oct 2007;20(10):1109-1114.
2. Ramachandran A, Snehalatha C, Joseph TA, Vijay V, Viswanathan M. Delayed onset of diabetes in children of low economic stratum–a study from southern India. Diabetes Res Clin Pract. Jan 1994;22(2-3):171-174.
3. Haines L, Wan KC, Lynn R, Barrett TG, Shield JP. Rising incidence of type 2 diabetes in children in the U.K. Diabetes Care. May 2007;30(5):1097-1101.
4. Feltbower RG, McKinney PA, Campbell FM, Stephenson CR, Bodansky HJ. Type 2 and other forms of diabetes in 0-30 year olds: a hospital based study in Leeds, UK. Archives of disease in childhood. Aug 2003;88(8):676-679.
5. Balakrishnan R, Webster P, Sinclair D. Trends in overweight and obesity among 5-7-year-old White and South Asian children born between 1991 and 1999. J Public Health (Oxf). Jun 2008;30(2):139-144.
6. Whincup PH, Gilg JA, Papacosta O, et al. Early evidence of ethnic differences in cardiovascular risk: cross sectional comparison of British South Asian and white children. Bmj. 2002;324(7338):635.
7. Krishnaveni GV, Veena SR, Hill JC, Kehoe S, Karat SC, Fall CH. Intrauterine exposure to maternal diabetes is associated with higher adiposity and insulin resistance and clustering of cardiovascular risk markers in Indian children. Diabetes Care. Feb 2010;33(2):402-404.
8. Ramachandran A, Snehalatha C, Yamuna A, Murugesan N, Narayan KM. Insulin resistance and clustering of cardiometabolic risk factors in urban teenagers in southern India. Diabetes Care. Jul 2007;30(7):1828-1833.
9. Vikram NK, Tandon N, Misra A, et al. Correlates of Type 2 diabetes mellitus in children, adolescents and young adults in north India: a multisite collaborative case-control study. Diabet Med. Mar 2006;23(3):293-298.
10. Ehtisham S, Crabtree N, Clark P, Shaw N, Barrett T. Ethnic differences in insulin resistance and body composition in United Kingdom adolescents. The Journal of clinical endocrinology and metabolism. Jul 2005;90(7):3963-3969.
11. Fischbacher CM, Hunt S, Alexander L. How physically active are South Asians in the United Kingdom? A literature review. J Public Health (Oxf). Sep 2004;26(3):250-258.
12. Feltbower RG, Bodansky HJ, McKinney PA, Houghton J, Stephenson CR, Haigh D. Trends in the incidence of childhood diabetes in south Asians and other children in Bradford, UK. Diabet Med. Feb 2002;19(2):162-166.