Abdominal Obesity Causes-Fat Depot Overflow
- One of the most important functions of adipose tissue is to provide sufficient storage for excess calories in the form of triglycerides. Insufficient storage leads to increased circulating free fatty acids and ectopic lipid deposition─ factors that are thought to result in insulin resistance that leads to diabetes.1
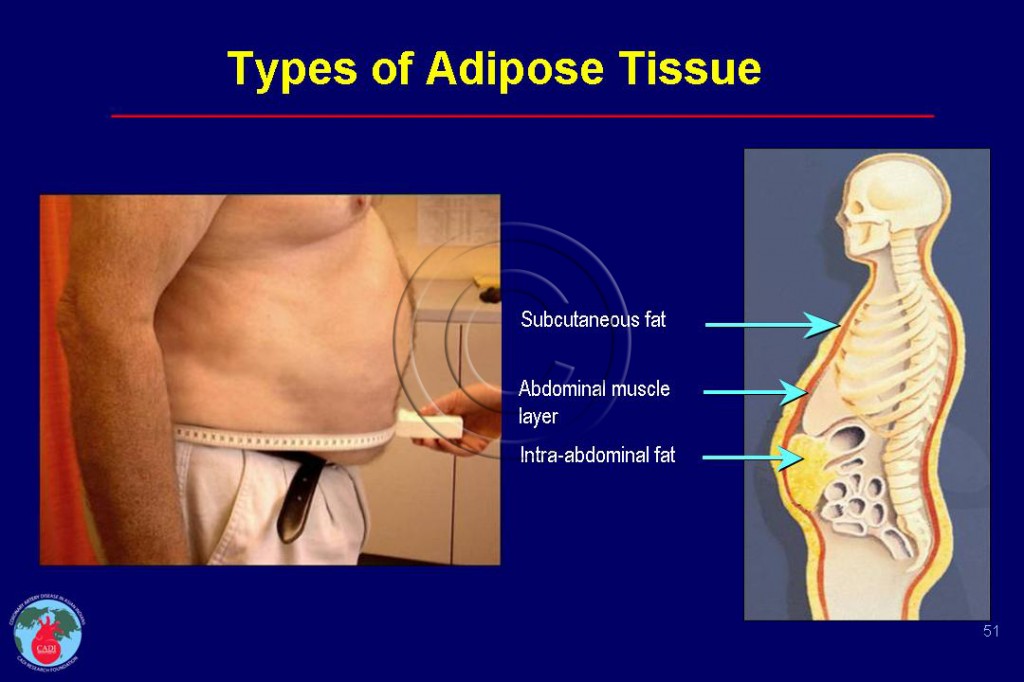
- The adipose tissue mass within human bodies can be divided into two different compartments─ subcutaneous, and visceral adipose tissue (see Figure 051).
- The subcutaneous adipose tissue compartment can be further divided into superficial and deep depots or compartments. The superficial fat depot is present throughout the body, and constitutes the vast majority of the adipose tissue in the lower limb and is relatively inert metabolically.
- With energy excess, the secondary adipose tissue compartments—the deep subcutaneous (mainly upper body) and the visceral adipose tissue compartments—become more prominent. 2 These two compartments are characterized by higher transmembrane fatty acid flux rates and thus are more closely linked to dyslipidemia and dysglycemia.
- The visceral fat tissue is an active endocrine organ involved in the dysregulation of metabolic inflammatory and hemodynamic processes.
- In some individuals, a disproportionate expansion of visceral relative to subcutaneous adipose tissue occurs. This manifests as an increased waist circumference (WC) and waist-to-hip ratio (WHR) and is associated with elevated risk of metabolic abnormalities. The mechanisms that support or limit the expandability of specific adipose tissue depots are not known.
- The storage capacity of adipose tissue is determined by the combination of adipocytes hypertrophy and hyperplasia, which give rise to expanded tissue mass. However, in humans the expansion of adipose tissue in response to excess caloric intake is not always uniform.
- The biologically inert primary fat depot (subcutaneous fat) is smaller among Asian Indians than Europids leading to more rapid overflow to the biologically active secondary fat depots, especially the visceral fat depot and this possibly explains the Asian Indian Phenotype.2
- Physical inactivity is an important contributor to abdominal obesity in every BMI category and both are independently associated with an increased risk of future coronary artery disease (CAD).3
- Energy-adjusted substitution of protein for an equivalent amount of carbohydrate can reduce abdominal obesity.4 Conversely, a high glycemic load (commonly observed in South India) can increase the risk of abdominal obesity. Substituting a modest amount of protein for carbohydrate (one chicken breast for two cups of rice) may reduce abdominal obesity.4
- Smoking is also positively related to abdominal obesity after accounting for body mass index (BMI). 4
Sources
1. Gealekman O., Guseva N, Hartigan C, et al. Depot-specific differences and insufficient subcutaneous adipose tissue angiogenesis in human obesity. Circulation. Jan 18 2011;123(2):186-194.
2. Sniderman AD, Bhopal R, Prabhakaran D, Sarrafzadegan N, Tchernof A. Why might South Asians be so susceptible to central obesity and its atherogenic consequences? The adipose tissue overflow hypothesis. Int J Epidemiol. Feb 2007;36(1):220-225.
3. Arsenault BJ, Rana JS, Lemieux I, et al. Physical inactivity, abdominal obesity and risk of coronary heart disease in apparently healthy men and women. International journal of obesity (2005). Feb 2010;34(2):340-347.
4. Merchant AT, Anand SS, Vuksan V, et al. Protein intake is inversely associated with abdominal obesity in a multi-ethnic population. J Nutr. May 2005;135(5):1196-1201.