Abdominal Obesity Overview
- The distribution of fat is more important than the total amount of fat in the body. Marked adverse metabolic consequences are seen with fat deposition in the abdominal region seen commonly in men and occasionally in older women. This is called Apple–type or central obesity, spare tire syndrome or simply abdominal obesity (see Figure 050)
- Although women have more fat than men, the fat is not deposited in the abdominal region but in the buttocks and thighs and is called gluteo-femoral (pear-type or gynoid) obesity (see Abdominal Obesity in Women).
- Abdominal obesity resulting primarily from visceral fat accumulation is a stronger predictor of dyslipidemia, diabetes, heart disease, stroke and deaths than general obesity.1-3
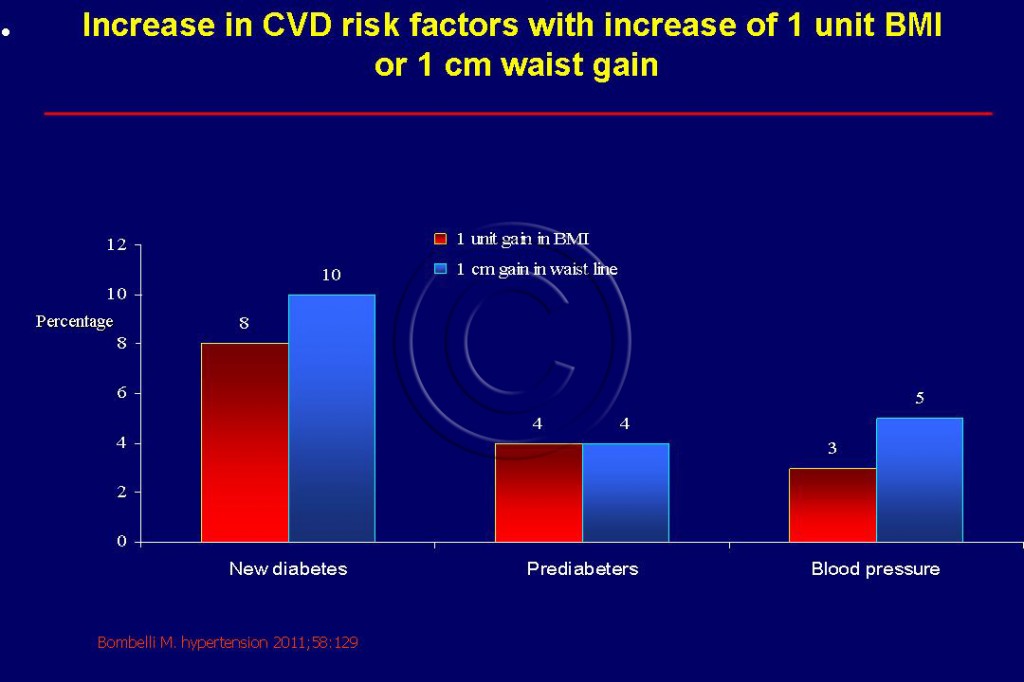
- A one cm increase in waist line confers a greater risk of diabetes, prediabetes and hypertension than a one unit of increase in BMI (5-7 lbs or 2-3 kg) as shown in Figure 114
- The simple and inexpensive measurement of waist circumference (WC) by a tape measure has been shown to be the best correlate of visceral fat mass as assessed by the expensive and time-consuming MRI scan.
- In some individuals, a disproportionate expansion of visceral adipose tissue relative to subcutaneous adipose tissue occurs. This manifests as an increased WC and waist-to-hip ratio (WHR) and is associated with elevated risk of metabolic abnormalities. The mechanisms that support or limit the expandability of specific adipose tissue depots are not known.
- The recognition of the significance of central obesity should not divert attention from the metabolic consequences of noncentrally obese individuals who need to reduce weight. Among Asian Indians, as in other populations, both body mass index (BMI) and WHR are related to coronary artery disease (CAD) risk factors in a graded manner; the maximum risk occurs in apple-shaped overweight and minimum in pear-shaped lean individuals.4 Therefore BMI should not be abandoned.
- Abdominal obesity, is not only more common, but also associated with greater dyslipidemia, metabolic abnormalities and higher insulin levels in Asian Indians than in Europids. (see Abdominal Obesity Indians)
FAQ
1. Where do you measure the waist circumference (WC)?
A. The iliac crest is currently recommended by the National Institutes of Health and National Heart, Lung, and Blood Institute. The World Health Organization recommends the use of the midpoint WC measurement. However, this method relies on the identification of 2 separate locations, the iliac crest and the lowest rib, and the need to calculate the midpoint of the distance between these 2 structures, which requires more skill and time than a measurement that relies on only 1 structure, such as the iliac crest.
2. What is the difference between adiposity and adiposopathy?
A. Adiposity can cause fat mass-related cardiovascular disease (CVD). However, excessive body fat does not always increase the risk of CVD. Adiposopathy (adipose-opathy) or sick fat refers adiposity causing adipose tissue anatomic and functional abnormalities that result in endocrine and immune derangements leading to diabetes, high blood pressure, and dyslipidemia. Adiposopathy provides an explanation for the increased metabolic abnormalities observed in Asians in general and Asian Indians in particular as well as most of the obesity paradoxes.
Sources
1. Enas EA. How to Beat the Heart Disease Epidemic among South Asians: A Prevention and Management Guide for Asian Indians and their Doctors. Downers Grove: Advanced Heart Lipid Clinic USA; 2010.
2. Franco O H, Massaro JM, Civil J, Cobain MR, O’Malley B, D’Agostino RB, Sr. Trajectories of entering the metabolic syndrome: the framingham heart study. Circulation. Nov 17 2009;120(20):1943-1950.
3. Arnlov J, Ingelsson E, Sundstrom J, Lind L. Impact of body mass index and the metabolic syndrome on the risk of cardiovascular disease and death in middle-aged men. Circulation. Jan 19 2010;121(2):230-236.
4. Prabhakaran D, Shah P, Joshi M, Puri S, Reddy K. Generalized obesity is also an important coronary heart disease risk factor in Indians. Indian heart journal. 1997;49:619.
5. Bays H. Statin safety: an overview and assessment of the data–2005. Am J Cardiol. Apr 17 2006;97(8A):6C-26C.